Painful Sex Specialist
Many conditions can cause painful sex symptoms. Maiden Lane Medical is skilled in diagnosing the causes of painful sex and helping New York City women get the treatment they need to relieve symptoms, restore confidence and feel better about their health.

STEPHANIE L.
What is dyspareunia?
Dyspareunia is the clinical term for genital pain just before, during, or after sexual intercourse. Painful intercourse varies significantly between patients.
For example, some patients experience pain during sexual entry, while others have discomfort during the act or a throbbing pain for hours after intercourse. In addition, some women may have pain when anything, including a tampon, is inserted into the vagina.


Dyspareunia
When should I talk to a doctor about painful sex?
Make an appointment to speak with your doctor at Maiden Lane Medical if you have recurrent painful sex. Identifying the cause of your discomfort and getting treatment can protect and improve your sex life, intimacy, and confidence.
What is vulvodynia?
Vulvodynia is classified as chronic pain or discomfort, which includes burning, stinging, irritation, or rawness of the female genitalia, specifically of the vulva. The word “vulvodynia” actually means “painful vulva.” This condition can severely impact the quality of life for affected women and may prohibit participation in sexual activity, physical exercise, and even social activities.
The condition is believed to be underreported because of its lack of visible symptoms and often a woman’s reluctance to talk about her symptoms. As many as one in six women may be affected by vulvodynia at some point in their life.
What is the cause of vulvodynia?
Vulvodynia does not have one set cause, but several factors can contribute to the development of chronic vulvar pain. For example, a history of recurrent vaginitis or vaginal yeast infections, as well as allergies, lupus, eczema, hip or back injury, or hormonal imbalance, can be some causes of this condition. In addition, people with vulvodynia are more likely to have other chronic pain conditions such as fibromyalgia, painful bladder syndrome, and irritable bowel syndrome.
Can anxiety cause vulvodynia?
Anxiety doesn’t necessarily cause vulvodynia or painful sex, but it does increase your risk of these issues. Depression, post-traumatic stress disorder, and a history of abuse can also increase your risk of painful sex and vulvodynia.
Is vulvodynia a neurological disorder?
Pain during sex has various potential causes. Vulvodynia and vestibulodynia are often caused by hypersensitivity or abnormal signals from the nerves. It is critical to have a thorough exam and testing with your trusted gynecologist to identify the root cause of your pain and the most effective treatment. ul
Have more questions?

What is vulvar vestibulodynia? (vulvar vestibulitis)
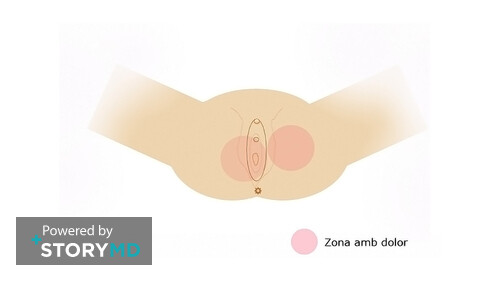
Vulvar vestibulitis is a form of vulvodynia in which a patient’s pain occurs in the vestibule or the area around the opening of the vagina. This condition can produce a burning sensation that may be persistent or arise mainly when pressure is placed on the vestibule. It is a common cause of sexual pain. It can be tested by a “q-tip test,” touching the tiny gland openings at the entrance to the vagina with a cotton-tipped applicator. If the patient suffers from vulvodynia, the area will be extremely sensitive.
What is the cause of vulvar vestibulitis?
The cause of vulvar vestibulitis is unknown, but inflammation, past infections, nerve injury, and hormonal changes are all believed to be contributing factors.
What is the treatment of vulvar vestibulitis?
There are several methods available to treat vulvar vestibulitis effectively. These include estrogen hormones, topical anesthetics, prescription medications that disrupt some nerve impulses, and physical therapy focused on the pelvic muscles. In more severe cases that do not respond to conservative treatments, vestibulectomy surgery may be recommended. This procedure involves removing some of the tissue of the vestibule to relieve symptoms.
Are there skin conditions that can cause vulvodynia?
Vulvar dermatoses, caused by dermatologic conditions, such as lichens sclerosis, are often present in the form of itching and burning. They are conditions associated with chronic vulvar pain, which can coexist with vulvodynia.
Can vulvar pain be more generalized?
Dysesthetic vulvodynia, or generalized vulvodynia, where symptoms occur throughout the vulvar anatomy, can occur constantly or intermittently. Patients have reported pain in the labia majora, labia minora, vestibule, clitoris, and inner thighs. Pressure to the vulva can trigger these symptoms but is not the only cause.
What is clitorodynia?
Clitorodynia is a form of vulvodynia in which the pain is concentrated in and around the clitoris. The area may feel sore and uncomfortable much of the time, mainly while exercising, wearing tight clothing, or having sexual intercourse. In some patients, sitting for long periods of time and dealing with stress can worsen the symptoms. This condition may be a result of trauma to the clitoral area or certain systemic illnesses, but in many cases, a cause is not found for clitorodynia.
Lifestyle changes such as wearing loose-fitting clothing, physical therapy, and over-the-counter pain medication may help some patients. However, prescription medication, topical pain relievers, and nerve block injections can be effective treatment methods for reducing pain for those with severe or persistent symptoms.
Vulvodynia
Have more questions?

What is coccydynia?
Coccydynia refers to pain and inflammation affecting the coccyx, or tailbone, which is located between the buttocks. Patients suffering from coccydynia may experience pain and tenderness on the tailbone, especially pronounced when sitting. Coccydynia is usually diagnosed through a physical examination, and in some cases, imaging scans to rule out other conditions. Treatment for coccydynia includes sitting in seats with sufficient padding and over-the-counter pain medication. Persistent cases of coccydynia may require cortisone injections, or in rare instances, surgery.
How is vulvodynia treated?
Treatment for vulvodynia may or may not cure the condition, but it does help to relieve symptoms.
Careful care of the vulva, avoiding toxins, and the use of cotton underwear, toilet tissue free of bleach, lubricants free of preservatives and chemicals, and non-perfumed soaps and creams can help mitigate symptoms and prevent flare-ups.
Trigger point injections can be used to insert a steroid medication as well as a numbing agent into the exact points where the pain is felt.
Topical agents, such as estrogen, can be applied daily to reduce pain.
Physical therapy or biofeedback treatments teach muscle control and allow patients to counteract pelvic muscle spasms.
A pelvic nerve block may be inserted to numb the nerves in the pelvic area.
BotoxⓇ injections may be used to relax spastic muscles and reduce tension pain in the region.
Is there surgery for vulvodynia?
Surgery is rarely recommended for vulvodynia and painful sex. Your doctor may recommend a vestibulectomy to remove tissue from the specific area where you feel pain. They only recommend this procedure when the pain is localized, and other treatments such as physical therapy and nerve blocks haven’t relieved your symptoms.
Are there other causes of painful sex?
Many factors can contribute to pain during sex. Some of the potential causes of your discomfort include:
- Insufficient lubrication
- Injury or trauma to the genitals
- Irritated or inflamed genital tissue
- Vaginismus (spasm in vaginal muscles)
- Pelvic inflammatory diseases
- Uterine fibroids
- Uterine prolapse
- Cystitis
- Ovarian cysts
- Scarring from previous surgeries
- Psychological issues
- Stress
Getting an accurate diagnosis is the first step in finding the proper treatment to relieve your pain. Pain during sex or persistent genital pain isn’t normal, and you shouldn’t ignore it.
How is the cause of pain during sex diagnosed?
The physicians at Maiden Lane Medical perform thorough exams and tests to identify the root cause of your discomfort. After reviewing your medical history and discussing your general health and symptoms, your doctor begins the physical exam. This included a pelvic exam, Pap smear, and lab tests. They may also suggest diagnostic imaging such as ultrasound or hysteroscopy to examine your reproductive organs.
Women's Health Specialists
Related Services
- Abnormal Pap
- Abnormal Periods
- Abnormal Uterine Bleeding
- Annual Gyn Exam
- Colposcopy
- Dense Breasts
- Dysmenorrhea
- Endometrial Polyps
- Fibroids
- Gynecology
- Hpv
- Mammogram FAQs
- Menopause Management
- Obgyn
- Ovarian Cysts
- Painful Sex
- Pelvic Pain
- Polycystic Ovary Syndrome
- Preparing for a Mammogram
- Uterine Prolapse
- Vaginal Infections
Don't know which doctor to choose? Let us help you.

STEPHANIE L.
What is vulvar vestibulodynia (vulvar vestibulitis)?
Vulvar vestibulitis is a form of vulvodynia in which a patient’s pain occurs in the vestibule or the area around the opening of the vagina. This condition can produce a burning sensation that may be persistent or arise mainly when pressure is placed on the vestibule. It is a common cause of sexual pain. It can be tested by a “q-tip test,” touching the tiny gland openings at the entrance to the vagina with a cotton-tipped applicator. If the patient suffers from vulvodynia, the area will be extremely sensitive.

Our doctors who provide this service
Emily Blanton, MD
Focused Practice Designation in Minimally Invasive Gynecologic Surgery
Janette Davison, MD
Focused Practice Designation in Minimally Invasive Gynecologic Surgery
Kenneth A. Levey, MD MPH FACOG FACS
Focused Practice Designation in Minimally Invasive Gynecologic Surgery
Schedule an appointment with Maiden Lane Medical today!
Are you ready to take control of your health? Look no further than Maiden Lane Medical!
Our esteemed medical practice offers specialized services in pap smears and other related health concerns.
Call us today to make an appointment online for expert diagnosis and personalized treatment!










