Vaginal Infections
Vaginal infections are a common concern for many women, causing discomfort and sometimes anxiety. In this comprehensive article, we will discuss vaginal infections and their various types, causes, symptoms, and treatments.
The most common things we call infections are mostly bacteria or yeast that usually reside in the vagina to some extent. With changes to the vaginal environment, some of the bacteria or yeast can overgrow and cause problems. We commonly refer to these overgrowths as “vaginal infections,” even though they are not true infections.
For expert care and personalized attention, consider scheduling an appointment with Maiden Lane Medical, a leading gynecology practice in New York City. Your health and well-being are our top priorities.

AMY
What is a Vaginal Infection?
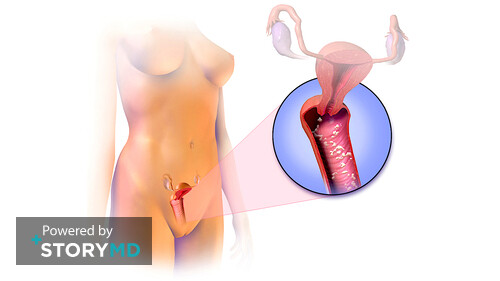
Vaginitis
A vaginal infection occurs when harmful bacteria, viruses, or yeast grow in the vaginal area, causing discomfort and other symptoms. Most vaginal infections are not serious and can be treated effectively. However, it’s important to understand the different types.
Types of Vaginal Infections
There are several different types of vaginal infections, each with its causes and symptoms. Here are some common vaginal infections:
- Bacterial Vaginosis: This is one of the most common vaginal infections/overgrowth and is caused by an imbalance of bacteria in the vagina. It often leads to a fishy odor, grayish-white discharge, and itching. Bacterial vaginosis is a type of bacterial infection.
- Vaginal Candidiasis: Also known as a yeast infection/overgrowth, this occurs when there is too much yeast called Candida in the vagina. Symptoms include itching, redness, and thick, white discharge.

- Common Sexually Transmitted Infections (STIs): Some vaginal infections are caused by STIs, such as trichomoniasis. This infection can cause itching, burning, and unusual discharge. Other common sexually transmitted infections that can affect the vaginal area include chlamydia and gonorrhea.
- Urinary Tract Infection (UTI): Although not a vaginal infection, a UTI can cause symptoms in the vaginal area, such as burning during urination, frequent urges to urinate, and pelvic pain. It is caused by bacteria entering the urinary tract.
What Causes Vaginitis?
Women’s Health: Infections
Vaginitis is the inflammation of the vagina that can cause itching, discharge, and pain. There are several causes of vaginitis:
- Yeast Infections: This type of infection happens when there is an overgrowth of yeast, called Candida, in the vagina. While many types of yeast can overgrow in the vagina and cause problems, candida is the most common.
- Sexually Transmitted Infections (STIs): Some STIs can lead to vaginitis. Common sexually transmitted infections like trichomoniasis, chlamydia, and gonorrhea can cause symptoms of vaginitis.
- Chemical Irritants: Products like vaginal sprays, douches, soaps, and scented tampons can irritate the vagina and cause vaginitis.
- Urinary Tract Infection (UTI): While not a direct cause of vaginitis, a UTI can sometimes be associated with vaginal irritation and discomfort.
What is the Difference Between a Yeast Infection and a Vaginitis?
Yeast infections and vaginitis are related but different conditions affecting the vagina. Yeast infections can be a cause of vaginitis, but not all vaginitis is related to yeast.
Yeast Infections
These are a specific type of vaginal infection caused by an overgrowth of yeast, particularly Candida. Symptoms include itching, redness, swelling, and thick, white discharge. Yeast infections are not sexually transmitted infections, although they can be triggered by factors like antibiotics, hormone changes, or a weakened immune system.
Vaginitis
This is a broader term that refers to the inflammation of the vagina, which can result from various causes. Vaginitis can be due to yeast infections, but it can also be caused by a sexually transmitted infection (like trichomoniasis, a common sexually transmitted infection), chemical irritants (such as vaginal sprays or scented products), or hormonal changes.
In summary, a yeast infection is a specific type of vaginitis caused by yeast overgrowth, while vaginitis is a general term for inflammation of the vagina with multiple possible causes, including bacterial infections, yeast infections, and sexually transmitted infections. Understanding these differences helps in diagnosing and treating the specific type of vaginal issue you may be experiencing.
Have more questions?
Is Vaginitis Contagious?
Vaginitis can be contagious, but it depends on the cause.
- Yeast Infections: Yeast infections are generally not considered contagious. They are caused by an overgrowth of yeast, usually Candida, which is normally present in the body. You can’t catch a yeast infection from another person.
- Bacterial Vaginosis: Bacterial vaginosis is a type of bacterial infection that is not typically considered contagious. It results from an imbalance of the natural bacteria in the vagina, and while it’s not spread through sexual contact, it can be associated with sexual activity.
- Sexually Transmitted Infections (STIs): Some causes of vaginitis, such as trichomoniasis, chlamydia, and gonorrhea, are sexually transmitted infections and are contagious. These infections can be spread through sexual contact with an infected partner.
- Chemical Irritants and Hormonal Changes: Vaginitis caused by irritants like vaginal sprays or hormonal changes is not contagious. These types of vaginitis result from individual reactions to chemicals or changes in hormone levels.
What Are the Signs of a Vaginal Infection?

Vaginal Yeast Infections

Bacterial Vaginosis
Signs and symptoms of a vaginal infection can vary depending on the type of infection, but here are some common symptoms to look out for:
- Itching: Persistent itching in the vaginal area.
- Burning Sensation: A burning feeling, especially during urination or sex.
- Unusual Vaginal Discharge: Discharge that is different from normal, which can be thick, white, yellow, green, or gray.
- Odor: A strong, unusual odor, often described as fishy.
- Redness and Swelling: Redness, swelling, or soreness around the vagina.
- Pain: Pain or discomfort in the vaginal area.
- Spotting or Bleeding: Light spotting or bleeding outside of your regular menstrual cycle.
If you experience any of these symptoms, it’s important to see a healthcare provider for a proper diagnosis and treatment. Vaginal infections are common and can usually be treated effectively with medication.
How is a Vaginal Infection Diagnosed?
Diagnosing a vaginal infection typically involves a few simple steps at the healthcare provider’s office:

- Medical History: The doctor will ask about your symptoms, sexual activity, and any previous vaginal infections. This helps them understand what might be causing the problem.
- Physical Exam: The doctor will perform a physical exam of the pelvic area to look for signs of infection, such as redness, swelling, or unusual discharge.
- Sample Collection: A swab of vaginal discharge may be taken. This is done gently with a cotton swab and is usually quick and painless.
- Laboratory Tests: The sample collected is sent to a lab to identify the cause of the infection. The lab can check for bacteria, yeast, or sexually transmitted infections.
- Additional Tests: Sometimes, a urine test might be needed to check for urinary tract infections or other issues.
These steps help the healthcare provider determine the specific type of vaginal infection you have, so they can recommend the right treatment. If you experience symptoms of a vaginal infection, it’s important to see a healthcare provider for proper diagnosis and treatment.
How is Vaginitis Treated?
Treating vaginitis depends on the cause of the infection:
- Yeast Infections: These are usually treated with antifungal medications, which can be in the form of creams, tablets, or suppositories. These medications help reduce the overgrowth of yeast and relieve symptoms.
- Bacterial Vaginosis: This type of vaginitis is treated with antibiotics that can be taken orally or applied as a cream. The antibiotics help restore the balance of healthy bacteria in the vagina.
- Sexually Transmitted Infections (STIs): If vaginitis is caused by an STI like trichomoniasis, it will be treated with specific antibiotics. It’s important to treat both partners to prevent reinfection.
- Chemical Irritants: If vaginitis is caused by irritants like vaginal sprays or scented products, stopping the use of these products usually helps. The irritation should go away once the source is removed.
Vaginitis doesn’t usually go away on its own and requires treatment to prevent symptoms from worsening or recurring. Maintaining good hygiene and avoiding irritants can help keep the balance of healthy bacteria in the vagina, which can prevent future infections.



Seek Expert Care at Maiden Lane Medical
Vaginal infections are common and can cause significant discomfort, but with proper diagnosis and treatment, they are typically easy to manage. Understanding the symptoms, causes, and treatments of various types of vaginitis can help you maintain your vaginal health and prevent future infections. If you’re experiencing any symptoms of a vaginal infection, don’t wait to seek help.
For expert care, schedule an appointment with Maiden Lane Medical, a trusted gynecology practice in New York City. Our experienced team is dedicated to providing comprehensive and compassionate care. Take control of your health today and contact Maiden Lane Medical for all your gynecological needs.
Women's Health Specialists
Related Services
- Abnormal Pap
- Abnormal Periods
- Abnormal Uterine Bleeding
- Annual Gyn Exam
- Colposcopy
- Dense Breasts
- Dysmenorrhea
- Endometrial Polyps
- Fibroids
- Gynecology
- Hpv
- Mammogram FAQs
- Menopause Management
- Obgyn
- Ovarian Cysts
- Painful Sex
- Pelvic Pain
- Polycystic Ovary Syndrome
- Preparing for a Mammogram
- Uterine Prolapse
- Vaginal Infections
Don't know which doctor to choose? Let us help you.

STEPHANIE L.
Our doctors who provide this service
Emily Blanton, MD
Focused Practice Designation in Minimally Invasive Gynecologic Surgery
Janette Davison, MD
Focused Practice Designation in Minimally Invasive Gynecologic Surgery
Kenneth A. Levey, MD MPH FACOG FACS
Focused Practice Designation in Minimally Invasive Gynecologic Surgery
Schedule an appointment with Maiden Lane Medical today!
Don’t forget to take advantage of Maiden Lane Medical’s annual gynecological exam service, now available at our new walk-in clinic in Murray Hill, NY. Ensure your continued health and well-being by scheduling your annual exam with us today!











